According to a recent study from Johns Hopkins Center for Health Security, "School Ventilation: A Vital Tool to Reduce COVID-19 Spread," ventilation improvements in K-12 schools are a cost-effective public health measure. A broad conclusion of this research is that investments in healthy air in schools offer far-reaching benefits in terms of both student health and academic achievement. "Improved ventilation may give children and school staff healthier indoor air quality for decades in the future, providing a healthier environment for non-pandemic times and potentially reducing risks in future infectious disease outbreaks," the report states.
Six evidence-based public health interventions
To help guide school administrators' investments, researchers with the Johns Hopkins Center for Health Security identified six evidence-based "building-level public health interventions" designed to "reduce the risk of COVID-19 transmission and promote long-term health and academic performance."
Hopkins investigators were quick to emphasize ventilation strategies that offer established efficacy standards. “School systems should not use unproven technologies such as ozone generators, ionization, plasma and air disinfection with chemical foggers and sprays,” reads the April 2021 Hopkins report. “The effect of these cleaning methods on children has not been tested and may be detrimental to their health.”
Instead, study authors recommend that “school systems should use only proven technologies for improving indoor air quality: Appropriate ventilation, HEPA filtration or ultraviolet germicidal irradiation.”
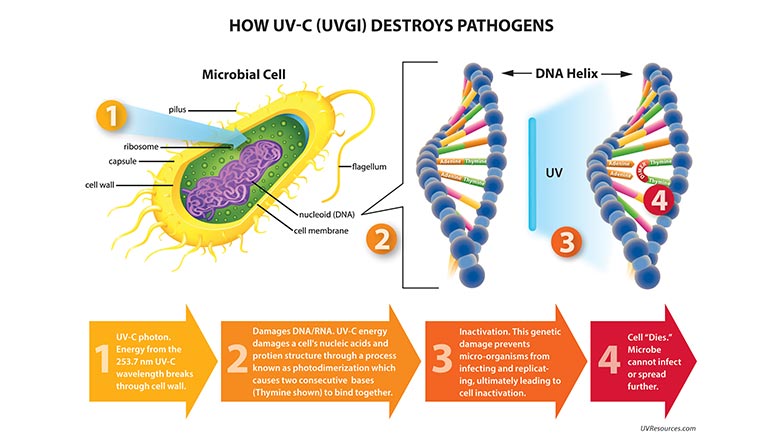
Ultraviolet germicidal irradiation (UVGI or UV C) does, in fact, offer nearly a century of proven efficacy in inactivating airborne and surface-bound viruses, bacteria and fungi (see Figure 1). Light in the 253.7 nm Germicidal UV C wavelength alters the protein structure in pathogens —DNA or RNA in viruses, bacteria or fungi — rendering the cell inactive and unable to replicate.

Germicidal UV C originally tested in schools
Ironically, UVGI technology was proven to inactive airborne pathogens in school classrooms nearly eight decades ago. In 1937, Harvard University epidemiologist William F. Wells installed Upper-Room UV lamps in suburban Philadelphia day schools to combat the measles virus. He then compared the measles infection rates of students who attended schools without UV C. Schools with the air-sanitizing equipment experienced a 13.3% infection rate compared to 53.6% for the control group.
Some 80 years later, researchers observed the SARS-CoV-2 virus to be highly susceptible to germicidal UV C irradiation. The Centers for Disease Control and Prevention (CDC) and ASHRAE recommend UV C as one technology that can "reduce the risk of dissemination of infectious aerosols in buildings and transportation environments."
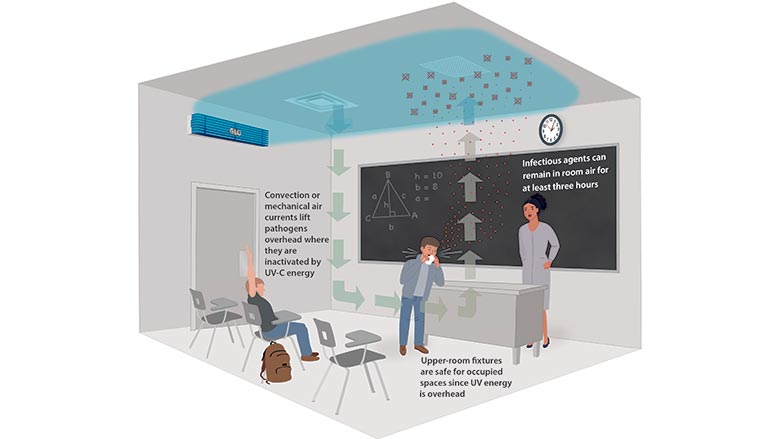
Known as Upper-Room or Upper-Air UVGI, the germicidal fixtures are wall-mounted near the ceiling, and non-reflective louvers angle the UV C energy upward and outward, away from room occupants (see Figure 2).
Upper-room UV C fixtures reduce pathogens
To demonstrate the importance of proper building ventilation and its impact on infection rates, UV Resources produced a computer simulation of viral particles spreading inside a typical classroom (Figure 2.1). Using computational fluid dynamic modeling, the video simulation shows how droplets from a sneeze can linger in a classroom, even with good airflow.

In a room with poor ventilation, enough droplets from a sneeze could linger in a cloud of particles even five minutes afterward, leading to possible "airborne transmission." Aerosols expelled during coughing, sneezing, or even talking can travel by air more than 30 to 40 feet. Upper-Room UV C fixtures can destroy microbes in a matter of seconds by creating an irradiation zone within the upper region of almost any space (Figure 2.4)
To demonstrate how Upper-Room UV C fixtures operate, UV Resources conducted a side-by-side comparison of two classrooms — one fitted with germicidal UV C fixtures and the other without.
To replicate particles generated by a sneeze or cough, droplets of four different sizes and velocities were dispersed in the computer model, using the center of a generic 34 foot by 27-foot classroom with 10 foot high ceilings (9,180 cubic feet). The simulation assumed four HVAC supply vents in the ceiling, a return air vent positioned above the "teacher" on the front wall, and a maximum capacity of 35 students.
Researchers believe that smaller droplets from a sneeze or cough of an infected individual remain in the air considerably longer than larger ones that fall almost immediately. That means ventilation systems could drive the viral particles throughout an entire classroom or other parts of the school and infect more people.
In addition, because fresh air ventilation helps control infectious particles by diluting space air with outside air, ASHRAE 62.1 "Ventilation for Acceptable Indoor Air Quality" specifies minimum ventilation rates and other measures to reduce adverse health effects for occupants. School classrooms typically require between four and 10 air changes per hour (ACH), and the computer modeling assumed six (6) ACH or recycling the classroom's air volume every 10 minutes. The higher the ACH rate, the lower the risk of spreading airborne disease.
The simulation demonstrates how convection or mechanical air currents lift pathogens overhead where they are exposed to UV C energy and inactivated in a matter of seconds. Because air movement is continuous, pathogen concentrations are further reduced with each subsequent pass of recirculated air ("multiple dosing") through the Upper-Room germicidal zone.
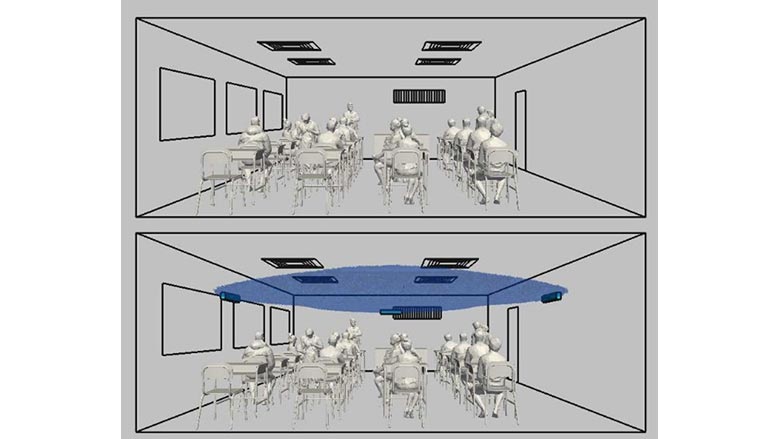
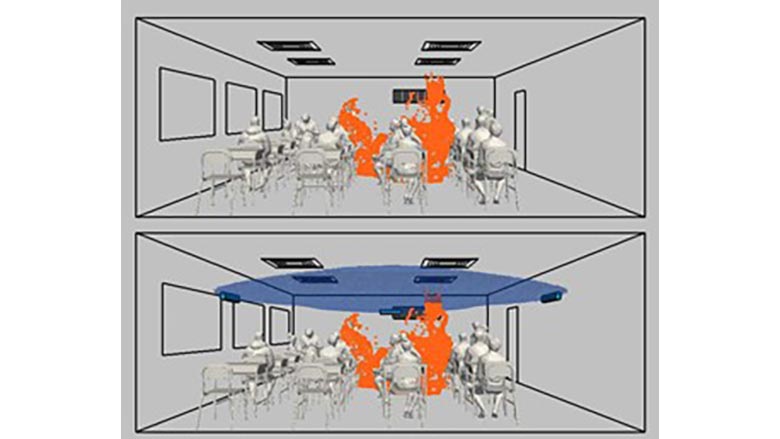

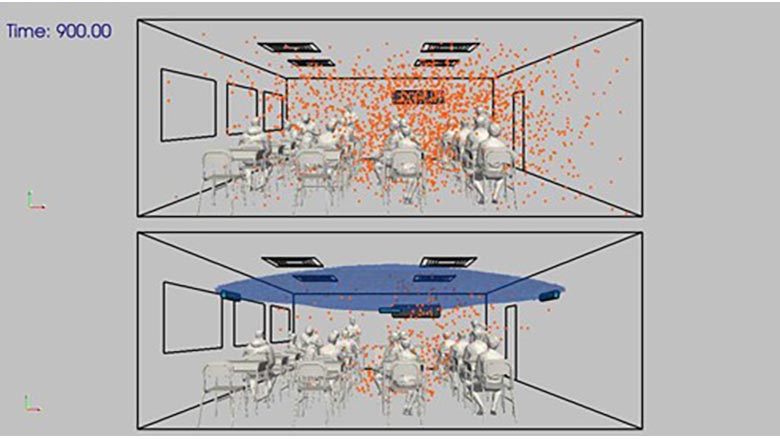
Contagious droplets can linger in spaces without UV C, such as the top classroom (Figure 2.5). Moreover, the longer a person is exposed to viral particles, the more likely they become infected and spread the disease further.
By eliminating airborne allergens, bacteria and viruses, Upper-Room UV C fixtures installed near a room's ceiling neutralize microbes as they circulate from the natural rise-and-fall of air currents.
Student health/performance outcomes driven by improved IAQ
According to a position paper from the LANCET COVID 19 Commission Task Force on Safe Work, Safe School and Safe Travel, researchers have found that better ventilation and air quality influence student health and academic performance outcomes.
To help put school air quality in perspective, 87 of 100 classrooms studied had ventilation rates below-recommended minimum standards, according to the LANCET Task Force paper, suggesting that nearly nine-of-every-10 classrooms lack sufficient healthy air.
“In addition to decreased airborne infectious disease transmission, research shows that ventilation and air cleaning improvements are likely to lead to improved academic performance (in particular reading and math performance), fewer missed school days for students, higher scores on cognitive function tests, and many benefits for teachers including decreased respiratory symptoms, increased teacher retention, and improved morale.”

Value of ventilation
LANCET Task Force researchers link schools with poor ventilation to above-average infection rates. While Upper-Room UVGI fixtures are not standard in classrooms, the CDC notes boosting room ventilation rates can reduce the number of infectious viral particles. “Ventilation interventions include opening windows, using fans, adding high-efficiency particulate air (HEPA) fan/filter systems, and adding Upper-Room ultraviolet germicidal irradiation (UVGI).”
The public health agency notes that UVGI kills airborne pathogens at their source (as contaminants are spread in room air), and fixtures are installed to prevent direct UV exposures to people in the room. Therefore, CDC recommends UVGI for indoor spaces with insufficient or no mechanical HVAC systems or spaces where adequate natural ventilation cannot be maintained year-round.
If adequate building ventilation and airflow mixing levels are not appropriate, concentrations of pathogens will multiply, raising the risk of infection for room occupants and viral spread. Even with proper ventilation, the possibility exists that HVAC systems can spread airborne pathogens beyond the source classroom.
What makes Upper Room UVGI particularly appealing is that it can be easily and affordably installed in existing classrooms. Unlike in-duct fixtures, these luminaries do not require knowledge of HVAC systems to install, and our product representatives can help guide in-house electrical or maintenance staff on proper fixture mounting and safety.
Upper-Room UVGI and in-duct UV fixtures are often used with other technologies in a multibarrier approach infection control strategy. Facility managers are encouraged to implement a layered approach incorporating multiple infection-control measures to ensure that any pathogen that cannot be removed by one method (e.g., filtration, cleaning) is inactivated by another (UV C).
Mitigating classroom infections
These recommendations align with long-standing industry guidance from ASHRAE in controlling airborne infections. For example, as part of its Position Document on Infectious Aerosols, developed by the Society's Environmental Health Position Document Committee, ASHRAE states:
“Dilution and extraction ventilation, pressurization, airflow distribution and optimization, mechanical filtration, ultraviolet germicidal irradiation (UVGI), and humidity control are effective strategies for reducing the risk of dissemination of infectious aerosols in buildings and transportation environments.”